What to Expect During a Hospital Stay
Have you ever sat in a hospital room listening to a doctor speak to you, thinking, “What the heck are they talking about?” Or “I have no clue what that means.” Your head is spinning and when the doctor asks if you have any questions, you can’t think of a single one and they leave the room. Hours later you have a list of questions to ask, but the doctor has left for the day.
Hospitalizations can be scary for everyone. The unfamiliar sights and sounds of the hospital can be uncomfortable for those who have not spent much time inside. After a cancer diagnosis, your family may be in and out of the hospital. Knowing what to expect during these stays can make the experience more comfortable and less confusing. This article will briefly overview some of the terminology, staff, and tests you may encounter during a hospital stay.
Common Medical Testing and Procedures
While in the hospital, your child will encounter many tests and procedures. While necessary, they can be uncomfortable, scary, and hard for your child to understand. To help them feel more comfortable, suggest the medical team demonstrate on your child’s favorite stuffed animal first.
Vital Signs
During your hospital stay, vital signs are routinely monitored. This helps your healthcare providers know how your child is doing. Below are commonly monitored vital signs.
Blood pressure measures the force or pressure of blood moving through the vessels of the body. It is measured by placing a cuff around your child’s arm (or leg if the arm is unable to be used) that gently squeezes the arm to take the measurement. You can explain this to your child by telling them the cuff will give their arm a quick hug.
Pulse oximetry. Another vital sign often measured is pulse oximetry, or pulse ox, which measures the amount of oxygen in the blood. This is done by placing a device (pulse oximeter) on a finger. It may resemble a plastic clip that opens and closes like a bird’s beak and is removed after the pulse ox is determined. A continuous pulse ox may be ordered by the doctor (such as after surgery). This device wraps around the finger like a Band-Aid and remains in place until removed.
Pulse. Heart rate, or pulse, is a measurement of how quickly the heart is beating. There are a variety of ways to measure heart rate, but while in the hospital, pulse is often measured with a heart monitor. The monitor displays the heart rhythm and the number of heartbeats per minute. To collect these stats, stickers with wires connected to the monitor are attached to your child’s chest.
Temperature. Your child’s temperature may be monitored using a thermometer. The temperature can be measured in the ear, mouth, armpit, rectum, or on the forehead.
Vein Access
If medications, chemotherapy, nutrition, or fluids are not administered in liquid or pill form, access to a vein, or blood vessel, is necessary. There are a few different ways to access the body’s veins.
Short-Term Vein Access
Intravenous Catheter (IV). An IV is a small catheter placed into a vein allowing medications and fluids to be given. Once an IV is placed, it typically remains in place for a few days. Fluids or medications can run through an IV intermittently or continuously. If the IV is placed where the arm bends, nurses may place a soft board on your child’s arm to keep it straight while the medication is infusing through the IV. Although the board may look uncomfortable, it is flexible and soft so as not to bother your child.
Long-Term Vein Access
Peripherally Inserted Central Catheter (PICC). A PICC line is another catheter that inserts into the vein and is a “step up” from an IV. It is placed in larger veins and can be used not only to administer medications, nutrition, and chemotherapy but also to draw blood (Mayo Clinic, 2023). This means fewer needle sticks for your child. PICC lines are usually placed in the upper arm and can remain in place for weeks to months. They can even remain in place when children are at home if cared for properly.
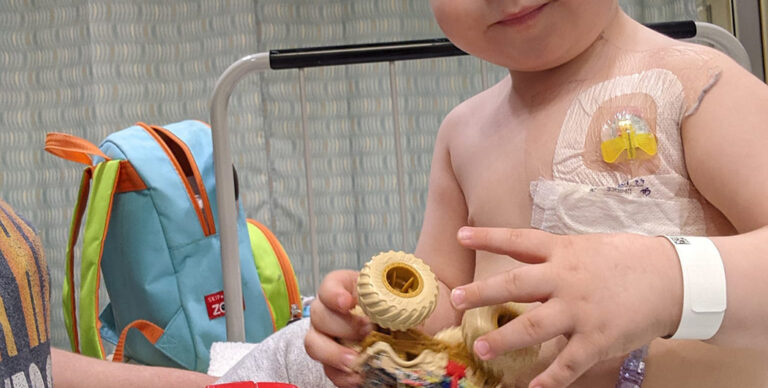
Implanted Port. An implanted port is another option for long-term vein access. It is a surgically implanted device that lives just under the skin (usually in the chest). The port connects to the veins so medications and chemotherapy can be administered (Cleveland Clinic, 2023). To access the port, a needle is placed through the skin into the center of the port. Once the needle is properly placed, it can remain there for days, and blood can be drawn from it. At discharge, the needle is removed, and your child can go home with the implanted port in place until the next time it is needed.
Hospital Staff
A large treatment team is assigned to your child during hospitalization and the frequent rotation of staff in and out of your room can be confusing. Let’s take a closer look at who you may encounter in the hospital.
Staff You Will Encounter Frequently
A pediatric nurse is the person you will probably see the most each day. They administer medications, perform assessments to see how your child is feeling, and assist with all needs throughout the day. A nurse is the frontline staff member who will identify changes or issues with your child, provide comfort on difficult days, and cheer with your family in times of happiness and success.
There is typically a second person assigned to your child for the shift, often called a patient care assistant. This person assists with care, performs blood work, checks vital signs, answers call bells, and more. Nurses and patient care assistants often work 12-hour shifts so there is less change throughout the day. Many hospitals have “rounding” protocols, where nurses and patient care assistants are required to check on their patients routinely. Frequent rounding leads to quick response time and allows the proactive identification of changes in your child.
Treatment Team
The pediatric oncologist is the cancer doctor who will determine the treatment plan for your child. Typically, the oncologist will round daily to check in, provide updates, and answer any questions. If necessary, a pediatric surgeon will join the team if surgery is needed to remove the cancer. The surgeon will be part of the team before, during, and immediately after surgery. After all surgical tasks are complete, your case may go back to the oncologist. An anesthesiologist administers and oversees the medication that helps your child go to sleep during surgery. A nurse practitioner or physician assistant may also be part of the treatment team. They work with the oncologist to create treatment plans and may check on patients daily while in the hospital.
Although this list of healthcare professionals is not all-inclusive, it is a start of who you may run into while spending time in the hospital.
Testing
To monitor where your child’s cancer is in the body and evaluate how treatment is working, testing is often called for. There are a large variety of tests that may be ordered by the doctor, depending on the type of cancer and treatment plan. Let’s explore some of the common tests you may hear about in the hospital.
Routine Tests
The most routine type of testing is blood work. Tons of information can be gathered from drawing blood, such as electrolyte levels, the presence of an infection, tumor markers, and more. Some blood work may even be ordered daily during hospitalization to look for improvements during treatment.
Another test that may be ordered is an ultrasound. An ultrasound uses sound waves to look at the inside of the body (American Cancer Society, 2024). You may know this test as the one pregnant women get frequently to see how their baby is growing. The test uses a small wand and gel that allows for easy movement along the skin. It shows internal imaging of the part of the body where the wand is touching.
Additional Tests
Three other tests may be ordered: x-ray, computed tomography (CT), and magnetic resonance imaging (MRI).
X-ray is often the first of these three types of imaging completed on a suspected area of cancer. This test is quick and similar to snapping a picture. Sometimes it takes longer to get into the right position for the “picture” than it does to capture the image.
A CT scan also uses X-ray technology but provides even more detailed pictures of internal anatomy than an x-ray (American Cancer Society, 2024). These tests can still be completed in a short amount of time like the x-ray.
An MRI is the longest of the studies and works by using a large magnet and radio waves to see the inside of the body (American Cancer Society, 2024). This test can take about thirty minutes to an hour. Children may be frightened by MRI machines as they are large and tube-shaped. Depending on the part of the body being looked at, your child may have to spend some time in a semi-enclosed space. Luckily, a stuffed toy or favorite blanket may accompany your child in the MRI machine, as long as there is no metal inside.
The part of the body being looked at will determine which of these exams is best, and more than one of these tests may be required.
Don’t Feel Uncomfortable Asking Questions
Despite hospital stays being overwhelming and full of uncertainty, they can also be full of healing and hope. Always remember to ask the nurses and healthcare providers questions. You and your family should feel comfortable and have a good understanding of the treatment plan. If you don’t, keep asking questions until you do.
References
American Cancer Society. (2024, May 28). If Your Child Has Cancer. https://www.cancer.org/cancer/types/cancer-in-children/if-your-child-has-cancer.html
Cleveland Clinic. (2023, January 31). What Is a Chemo Port? https://my.clevelandclinic.org/health/treatments/24663-chemo-port
Mayo Clinic. (2023, June 3). Peripherally inserted central catheter (PICC) line. https://www.mayoclinic.org/tests-procedures/picc-line/about/pac-20468748#:~:text=A%20peripherally%20inserted%20central%20catheter,be%20placed%20in%20your%20leg